Arkansas
Success Stories
Wife and Caregiver Shares Story on Caring for Her Husband After a TBI, Using Telemedicine

THE ACCIDENT
As the COVID-19 pandemic continues to affect the healthcare system, telemedicine has expanded and evolved to assist patients and families in need including the Tolerson family. On March 21, 2020, Alex Tolerson experienced a seizure while driving, causing him to swerve off the road, hit a tree, spin around, and slam into a brick wall. After paramedics extracted Alex from his car, EMS airlifted Alex to the University of Arkansas for Medical Sciences (UAMS) in Little Rock, Arkansas. There, he was diagnosed with a grade III severe diffusion axonal injury, subarachnoid hemorrhaging, frontal lobe damage, lesions in his brain stem and his corpus callosum, C2 facture, lesion to the left side of his forehead, and broken orbital floor of his left eye. Alex’s accident had left him with a Traumatic Brain Injury (TBI). Surgery was not required, but doctors had to intubate Alex, and place him on a ventilator in a state of unconsciousness. Because this major accident occurred during the beginning months of the pandemic, the Tolerson family experienced even more hurdles for Alex’s care.

COVID-19 IMPACT ON THE TOLERSON FAMILY
Vida Tolerson, Alex’s wife and caregiver, was able to visit with her husband for two hours before he moved to the Intensive Care Unit. After that, she was no longer able to visit him because of restrictions due to the pandemic. Alex’s stay in the hospital lasted until for over a month. All Vida could do during that time was call the hospital to get updates on her husband’s health until he could be moved to a long-term acute care facility (LTAC). At the LTAC, COVID-19 restrictions again prevented Vida from being at her husband’s bedside. She not only wanted to check on her husband, but also to know how to care for someone with a TBI for when Alex was able to come home. Vida spent time online researching and learning the best ways to care for a TBI patient until she could learn from his healthcare team at the LTAC.
Once Alex was home, Vida dove into caring for him. She quickly learned different therapies, techniques, and massages. It was difficult at first to get into a schedule and to know what he needed. In the beginning, Alex would open his eyes sporadically; he was agitated and storming[i] a lot. After that, the Tolerson family began to find their rhythm. Things got easier. Alex would have his days where he was unresponsive or would become over stimulated, but the family learned to adjust to Alex’s new cues. While the family is making great strides with Alex’s care, the pandemic has created major barriers for him and his family.
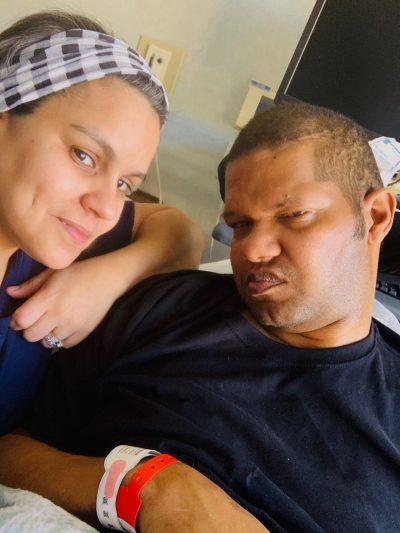
TELEMEDICINE INTERVENTION
The Tolerson family lives an hour and a half outside of Little Rock, and away from Alex’s healthcare providers. In order to provide him with appropriate care, limit travel time, and lessen the risk of a COVID-19 pandemic, UAMS worked with the Tolerson family to setup telemedicine video-calls with Alex’s physiatrist. This alternative method of care saved Alex from the challenges of a trip-by-ambulance to appointments at the Little Rock clinic. The first telemedicine assessment was enough for the physiatrist to take him on as a patient, change medications, change some therapies, and start moving forward with recovery. Since then, the Tolerson family has participated in three telemedicine appointments and Alex has progressed to a state known as minimal consciousness. Through the video capabilities of telemedicine, the healthcare providers were able to see Vida and Alex in their everyday environment.
I don’t know where we would be without telemedicine–it was great!
Vida Tolerson

One of the most important factors of telemedicine is being able to review Alex’s medications. His healthcare providers reviewed his medications and made a change from one that was keeping him more sedated, to one that was still therapeutic but would allow him to be more alert. Now, after just three telemedicine visits, Alex is moving onto the next stage of his recovery and is starting to emerge a bit more. He can reach for things now, his contractures are good, he opens his hands completely, and Alex’s cervical collar was able to come off. Vida explained that the telemedicine visits helped her better care for her husband. She is able to explain visually any questions or concerns to his healthcare team. “The telemedicine visit allows that one-on-one interaction with the patient that you would never get just picking up the phone and calling,” she explained. Nothing is up for interpretation; the healthcare providers are able to see exactly what Vida is talking to them about. Although communicating through telemedicine is not a physical face-to-face interaction, you are still able to see, hear, and interact with one another.
The talk is to bring Alex in [to the clinic] in a couple of weeks for rehab and I don’t think that would have happened without telemedicine.
Eddie Williams, RN, BSN, CBIS, Nurse Educator, UAMS IDHI Trauma
[1] Storming: Patient’s body’s response to the stress of a severe TBI that can include symptoms such as elevated heart rate, high temperatures, rigid body postures, profuse sweating, hypertension, and fever.
[1] Physiatrist: physical medicine rehabilitation doctor focused on disorders of consciousness. (Some may call this a vegetative state or persistent comatose state.)
Contributors: Eddie Williams, RN, BSN, CBIS, Terri Imus, RN, BSN, Kim Lamb, MS, Kristen Alexander, MPH, MPS
