Fact Sheets
A Provider’s Guide: Telehealth Reimbursement Coverage in Hawaii During COVID-19
Rapid developments with the COVID-19 pandemic have resulted in a set of broad expansions of telehealth policy, including key changes to both public and private payer payment policies, at least for the duration of this emergency period. These changes include a CMS waiver dramatically broadening Medicare telehealth payment policies under HR 6074, enacted March 17, 2020; HR 748, enacted March 27, 2020; and federal action to periodically waive enforcement of HIPAA sanctions.
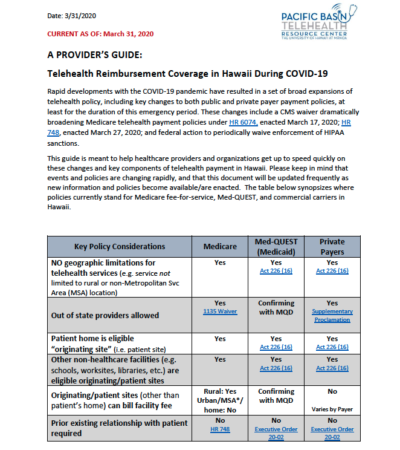
This guide is meant to help healthcare providers and organizations get up to speed quickly on these changes and key components of telehealth payment in Hawaii. Please keep in mind that events and policies are changing rapidly, and that this document will be updated frequently as new information and policies become available/are enacted. The table below synopsizes where policies currently stand for Medicare fee-for-service, Med-QUEST, and commercial carriers in Hawaii.